Not Enough Doctors Recommend the HPV Vaccine — And It Sends a Harmful Message About Sex
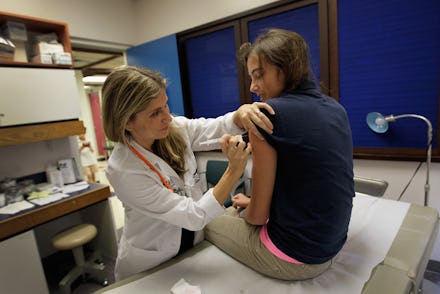
Human papillomavirus (HPV), a group of more than 150 related virus strains, is the most common sexually transmitted infection in the United States. Transferred by intimate skin-to-skin contact, HPV infection can lead to an array of negative and entirely unpleasant health issues, ranging from genital warts to cancer.
Luckily, there's a vaccine to prevent all of that — but too few doctors are recommending it to their patients.
According to a report out this week in the journal Pediatrics, a troubling number of doctors are failing to push for the HPV vaccination among patients under the age of 16, despite the fact that the American Academy of Pediatrics recommends girls and boys get the vaccine when they're 11 or 12, before they become sexually active.
But a survey of 600 doctors found that more than one-third don't actually recommend it, according to the Associated Press.
The reason? They don't want to talk about sex.
The study, which included 582 pediatricians and family physicians, asked doctors about their 11- and 12-year-old patients. Although most physicians included in the survey (84% of pediatricians and 75% of family physicians) said they almost always discuss the vaccine with these patients, a third of doctors did not strongly recommend it to them. These doctors were the ones who assumed or feared that parents wouldn't approve of giving the shot to preteens. According to the AP, and another Pediatrics study, one-third of teens have had sex by the time they turn 16.
Fewer than 2% of adolescents, however, have had sex by their 12th birthday, according to Guttmacher. Then the rate shoots up dramatically; 16% have had sex by age 15. That's part of why AAP recommends the HPV vaccine for preteens, says Dr. Allison Kempe, a professor of pediatrics at the University of Colorado School of Medicine and lead author of the new study.
"The problem with [recommending the vaccine later] is that the vaccine is maximally effective if given before sexual activity, and the immune response to the vaccine is better in early adolescents rather than later," Kempe told Mic.
Kempe and her co-authors believe doctors and patients would both benefit from a clearer understanding of why it's better to administer the vaccine at an earlier age, especially given the current lag in vaccination rates. The Centers for Disease Control and Prevention estimates that 60% of girls and just over 40% of boys between the ages of 13 and 17 have gotten at least one dose of the recommended three to complete HPV vaccination.
In short, a lot of teens haven't.
Given the vaccine is recommended for all preteens, current vaccination rates are considered too low. The CDC attributes this to a "knowledge gap" among parents, but it's also partly attributable to the doctors. As a Harvard Medical School study from October 2015 found, "The single biggest barrier to increasing HPV vaccination is not receiving a health care provider's recommendation," according to study leader Melissa Gilkey.
The misinformation all seems to be rooted in our culture's deeply embedded antipathy toward talking to kids and teens about sex. "Discomfort talking about sex appears to be a more salient factor" than safety or efficacy concerns, Gilkey told NPR.
It's unclear whether or not sound science and basic logic can overcome long-lasting misconceptions about what happens when you teach kids about sexual health (hint: It doesn't make them have sex any sooner, and actually might contribute to delayed sexual activity). Medical professionals aren't immune from internalizing stigma about sex: Physicians and pharmacists alike have been known not only to buy into myths about young people's sexuality, but to perpetuate them as well.
Not bringing up the HPV vaccine because it might mean having an uncomfortable conversation — or confronting the reality of teen sexuality – isn't just bad medicine. It contributes to a culture of shame and silence about sex and sexual health. It could also be putting their lives at risk.