Studies suggest that Pfizer is no longer the cooler vaccine
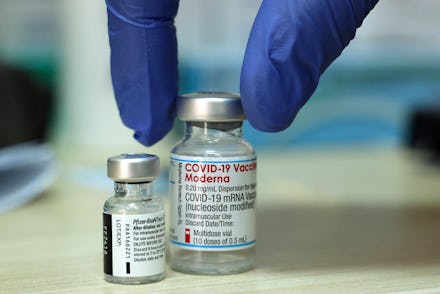
After I got my Pfizer shot last spring, I showed my vaccine card with pride wherever I went: I felt like I had the Comme des Garçons of inoculations and everybody needed to know. For some time, people I knew on social media also propagated the belief that Pfizer was the Hot Person Vaccine, slightly more effective than the others and with no side effects. But recent studies have found that over time, it is actually Moderna’s vaccine that might better protect people from severe illness, according to the New York Times.
In fact, the efficacy against hospitalization of the Pfizer vaccine fell from 91% to 77% after just four months, according to the CDC. Meanwhile, Moderna’s ability to stave off hospitalization remained the same, at 93%. But experts have made it extremely clear that there’s no need to freak out now if you got Pfizer, because both vaccines remain extremely effective at preventing severe illness.
Now, I know it’s easy to jump to conclusions after seeing the numbers, the results of these studies don’t automatically mean that you’re more likely to get sicker if you got Pfizer instead of Moderna. That’s because there are several factors at play, including the fact that Pfizer was authorized before Moderna, and given to older adults and healthcare workers first.
Because the immune response diminishes faster in older adults, a decline in protection seen in a group of primarily older people vaccinated with Pfizer could make the vaccine appear less effective this far into the pandemic, according to the Times.
But there is still some evidence that Moderna has been better in general at preventing infections against the Delta variant, which now accounts for a staggering 99% of all U.S. cases. While both vaccines work similarly, research conducted over the summer found that Moderna recipients were nearly 30% less likely to experience a breakthrough infection.
Per the Times, a handful of studies have found that Moderna caused the immune system to churn out more antibodies. In fact, one study that’s awaiting peer review has found that Moderna produced almost double the amount of antibodies than Pfizer did, according to Bloomberg.
But the amount of antibody production has more to do with an individual’s immune response than it does with the vaccines themselves. Even low levels of antibodies are enough to fight an infection and it’s worth remembering that most vaccines, including the ones for flu, are between 40% to 60% effective.
Whatever the reality of each COVID vaccine’s efficacy may be, the CDC report has inevitably upped the heat on conversations around booster shots and who should get them first. If Pfizer’s protection drops off even faster in older and immunocompromised people, then those who received the vaccine months ago could be ushered to the front. Regardless of what happens, it’s essential to remember that both vaccines remain extremely successful at what they were ultimately designed to do: prevent people from being hospitalized with or dying of COVID.