Alzheimer’s is already a serious problem in the US — and numbers will double by 2060
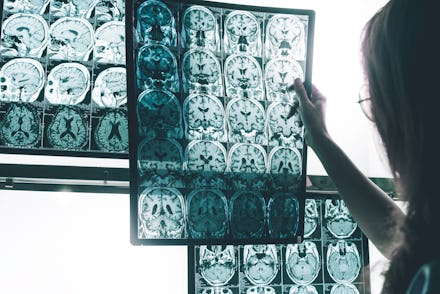
The number of people at risk for Alzheimer’s disease is rapidly rising in the United States, and everyone — young and old — should pay attention.
More than 93,000 people in the U.S. died from the disease in 2014, according to the Center for Disease Control and Prevention — which far exceeds the number of people who died from diabetes mellitus, influenza, pneumonia, Parkinson’s or suicide. Meanwhile, about 5.5 million Americans are thought to have the disease (numbers vary, depending on the source).
Now, scientists believe the issue is about to get much worse: A recent study from the University of California, Los Angeles, projects that the number of Americans with Alzheimer’s or “mild cognitive impairment” (early symptoms of the disease) will more than double by 2060.
That comes out to about 15 million people.
“What’s really driving that is a change in the age structure of our population. We’re getting older, and that profile is going to see a lot more Alzheimer’s disease,” Ron Brookmeyer, a professor of biostatistics at the UCLA Fielding School of Public Health, said by phone.
“This was the first study that has actually quantified the number of people who not only have Alzheimer’s dementia — which is the late stage of the disease — but also quantified the earlier stages,” he added.
Brookmeyer and his colleagues estimate that about 47 million people in the U.S. currently have evidence of preclinical Alzheimer’s. These signs aren’t exactly noticeable symptoms, but instead biomarkers detected by doctors — such as the buildup of beta-amyloid protein fragments in the body or brain neurodegeneration.
However, not all of those 47 million people will actually get Alzheimer’s.
“Only a fraction of them would,” Brookmeyer said. “The natural [progression] of this disease is very long and it takes decades. Many people’s natural lifespans will not be long enough for the disease to progress to the point where they actually experience dementia.”
In other words, a 65-year-old woman with early signs is much more concerning to medical professionals than a 90-year-old man. In that scenario, the woman would likely have more time for the disease to progress.
What is Alzheimer’s disease?
The National Institute on Aging — part of the U.S. Department of Health and Human Services — defines Alzheimer’s disease as an “irreversible, progressive brain disorder that slowly destroys memory and thinking skills.” A mild form of the disease includes symptoms such as depleted energy and motivation, loss of recent memories, issues with language and coordination, mood swings or depression and trouble driving (particularly with navigation). Eventually, the disease can progress to the point of making simple tasks difficult or impossible to carry out.
Contrary to popular belief, Alzheimer’s doesn’t exclusively affect senior citizens. A rare, early-onset form of the disease can affect people between their 30s and mid-60s, but the majority of diagnoses involve people whose symptoms appear in their mid-60s or later.
But no matter the age, full-blown Alzheimer’s disease can significantly affect lives. Not only does it emotionally impact patients and the people close to them, but it costs the U.S. health care system and loved ones heaps of money.
Many patients need intensive care from a nurse or assistant, for instance — and that service costs an average of $43,539 annually for a single patient to live in a basic assisted-living facility, according to the Alzheimer’s Association. A semi-private room in a nursing home can cost an Alzheimer’s patient an average of $82,125 a year.
So, as numbers of Alzheimer’s patients increase, so will the costs. The UCLA study found that an estimated 4 million Americans will need such aid by 2060, and Brookmeyer believes that this the nation should plan to have a healthy supply of resources for various stages of the disease.
“It gives you an idea of the level of care that we would need. These are big numbers and big increases compared to what we’re seeing now,” Brookmeyer said. “The impact of this disease would be huge.”
More intervention is needed, experts say
For now, scientists aren’t certain what causes the disease, but a combination of “genetic, lifestyle and environmental factors” are thought to contribute to its rise. Much of the science is preliminary, and some studies have suggested that head trauma, obesity, high blood pressure, smoking and a lack of fruits and vegetables in one’s diet are linked to the disease. Women are also more likely to develop Alzheimer’s.
Brookmeyer says that there is “accumulating evidence” that cognitive training, blood pressure management and exercise “may slow the progression of the disease.” But much of Alzheimer’s research today is still trying to figure out how to best detect the disease at different stages, then when and how to best treat each one.
“We need to develop interventions that work all along the continuum of the [disease’s development],” he said. “It’s a tall order, but that’s currently where the field is and that’s where the research needs to move forward.”